Funciona con las nuevas variantes
Las mutaciones de la proteína «S» del virus afectan a muchos test, dejándolos inservibles, ya que no pueden detectar las nuevas variantes.
Nuestro test es capaz de detectar todas las nuevas variantes incluyendo las variantes Británica (VOC-202012/01), Sudafricana (501Y.V2), Brasileña (P.1) y la más reciente de Uganda (A.231)
Alta sensibilidad
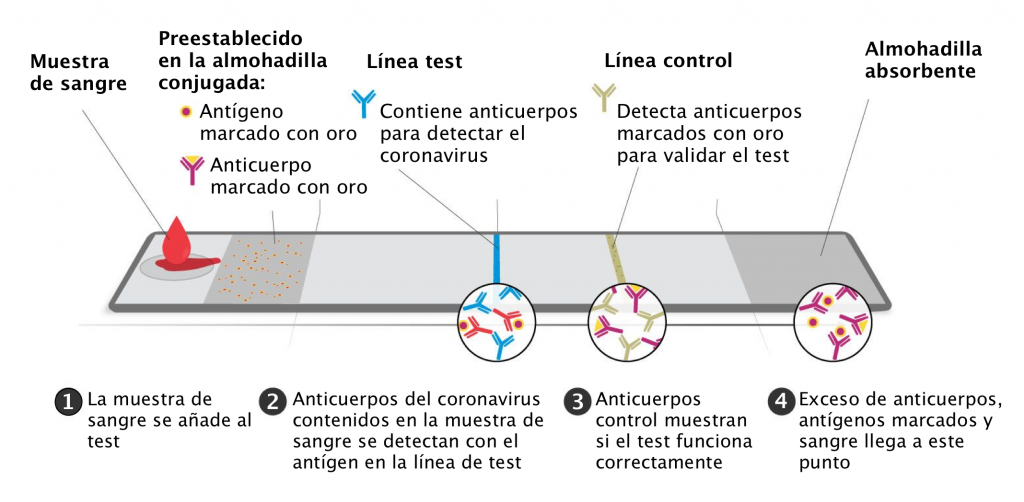
Gracias a los antígenos usados, la tecnología de oro coloidal por flujo lateral detecta la presencia de anticuerpos contra el coronavirus (SARS-CoV-2) aunque no se presenten síntomas.
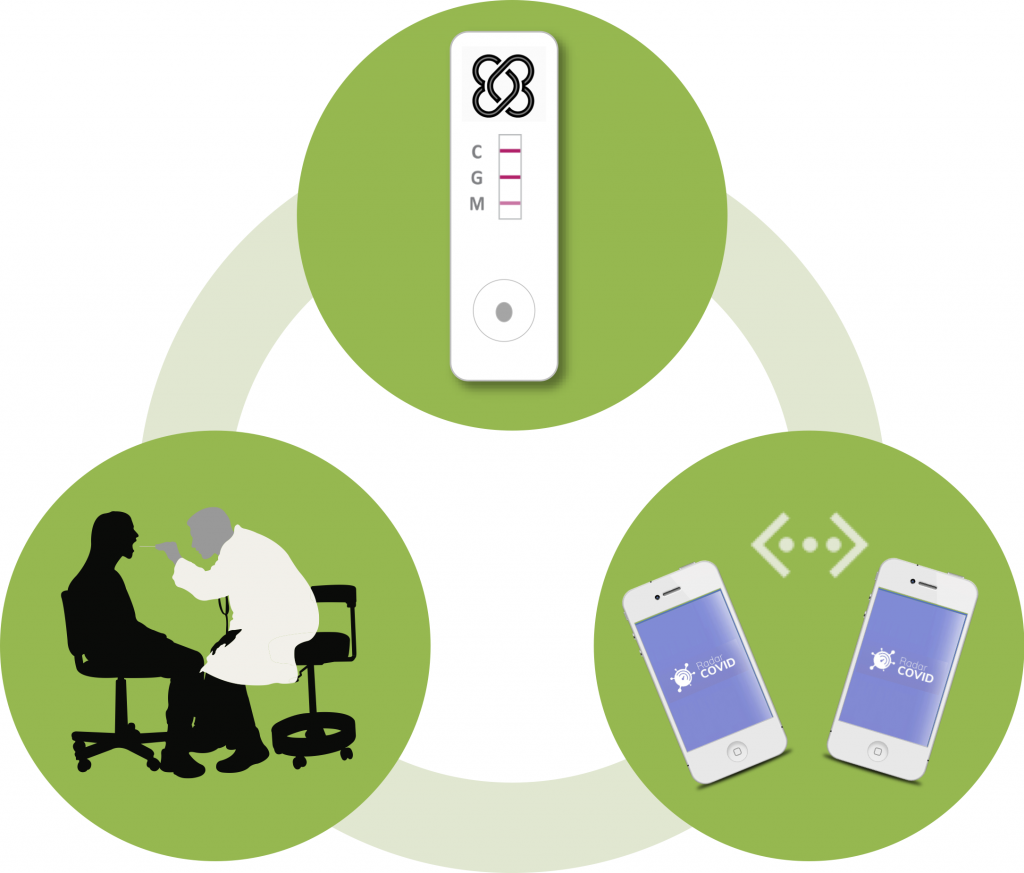
Las pruebas rápidas son un complemento clave para controlar la Covid19
La combinación del serocribado con los test antigénicos y el rastreo digital proporciona el mejor complemento a las vacunas, permitiendo localizar los portadores y sus posibles contactos, reduciendo la circulación de virus y evitando la aparición de nuevas variantes.
Datos seguros y anónimos
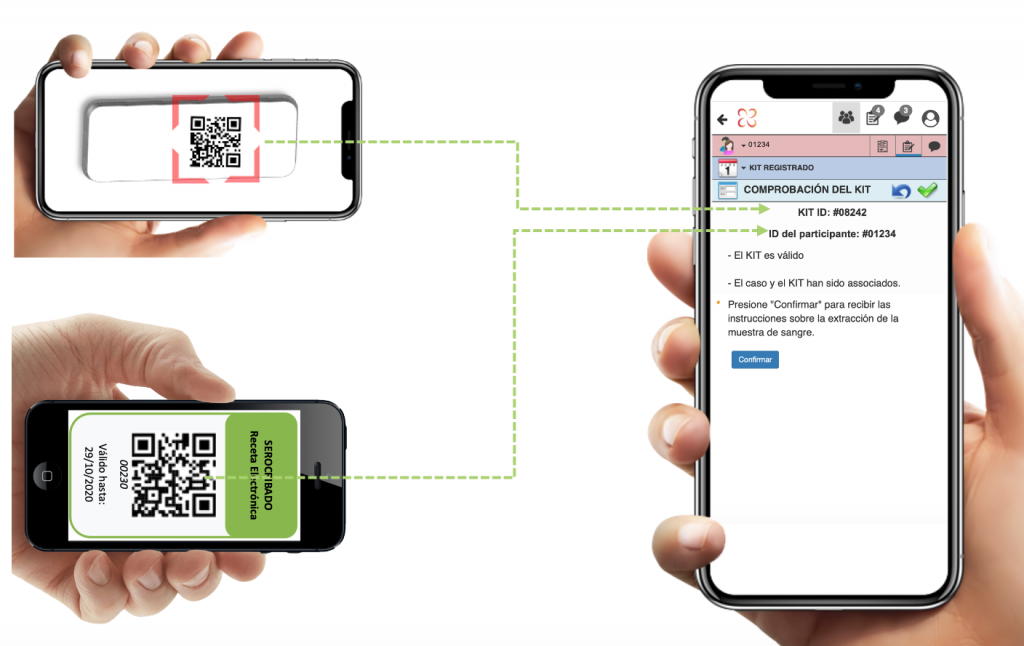
La plataforma de Linkcare permite crear recetas eletrónicas, procesar los QR de los tests y asignarlos a un participante y monitorizar el tiempo para leer los resultados del test. Todo esto anonimizando los datos.